By Chris Faubel, MD —

In pain medicine we treat a myriad of conditions with various injections (epidural steroid injections, peripheral joint injections, trigger point injections, prolotherapy, sympathetic blocks, botulinum toxin, etc.). One thing that all of those procedures have in common, is a needle.
Whether it’s the needle itself, or the acidic lidocaine, our injections have some degree of pain.
Besides using the smallest diameter needle possible for the respective procedure, there are other methods we can employ to eliminate or minimize the injection pain.
Vapocoolant sprays
- Cools the skin to a point where the nerve conduction velocity of C fibers and A-delta fibers have reduced ability to transmit injection site pain to the brain. [1]
- Mechanism of action:
- The evaporation of the liquid cools the liquid stream by the time it impacts the skin. The liquid on the skin continues to evaporate and remove heat from skin resulting in the rapid decline of the skin temperature. [2]
- Used since the 1940’s
- Made principally by the Gebauer company out of Cleveland, Ohio
- Directions: spray until the skin starts to blanch (turn white)
- Time needed varies, but is usually 5 seconds or less
- Can be used on open skin
- Great for reducing or eliminating the sting of the needle stick, but does nothing to augment the burning sensation that accompanies subcutaneous lidocaine infiltration.
- Are these products sterile?
- Many people wonder about this, because they’re sprayed directly over the injection site just prior to needle insertion.
- The major manufacturer has this to say on their website:
- Fluori-Methane spray
- A chlorofluorocarbon, which have been banned since 1990 because of their deleterious ozone effects
- Was used by Travell and Simons for treating myofascial pain
- Has been replaced by “Gebauer’s Spray and Stretch”
- Gebauer’s Spray and Stretch
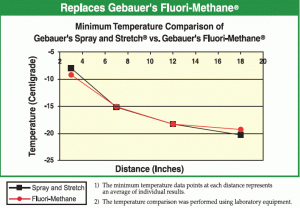
Gebauerco.com - Fluoropropane and fluoroethane mixture
- Equivalent cooling effect as Fluori-Methane (see chart to right)
- Ethyl Chloride spray
- Most common one used before injection
- Very flammable
- Can vs Bottle
- The bottle needs to be turned over completely and the lever squeezed fully to get a good stream; otherwise it trickles out and is wasted.
- The bottle is more expensive
- The can comes in stream and mist spray patterns for more variety (personal preference)
- Pain Ease
- Another product by Gebauer
- Active ingredients are 1,1,1,3,3- Pentafluoropropane and 1,1,1,2-Tetrafluoroethane
- NOT flammable; NOT bad for ozone
- Pain Ease, Ethyl Chloride, and Spray and Stretch all have equivalent cooling profiles
EMLA cream
- Lidocaine 2.5% and Prilocaine 2.5%
- Directions
- Apply a thick layer of cream and cover with an occlusive dressing (duoderm, tegaderm)
- Down side
- Have to wait 30-60 minutes after applying the cream
Ice cubes
- Problem: cumbersome and messy
Sodium bicarbonate buffering of lidocaine
- The burning sensation of lidocaine being injected into the patient’s skin may quite possibly be the most painful aspect of the injection process.
- Lidocaine is more acidic than human tissue, and this is believed to be the reason for the burning sensation.
- Bicarbonate neutralizes the acidic lidocaine –> Less pain
- Directions
- Add 1ml of 8.4% sodium bicarbonate to a 10ml bottle of lidocaine (with or without epinephrine)
- Note: the buffered lidocaine decreases the effectiveness of the epinephrine. But since we rarely use epinephrine with our injections in pain medicine, this is less relevant to us.
- The buffered lidocaine has also been shown to have even more antibacterial activity [3]
Warm the lidocaine and inject slowly
- Body temperature lidocaine produces less pain than room temperature [4]
- One study found that the rate of administration of lidocaine had a greater impact on the perceived pain of lidocaine infiltration than did buffering. [5]
————————————————————————————-
REFERENCES:
1 – Weiss RA, Lavin PT. “Reduction of Pain and Anxiety Prior to Botulinum Toxin Injections With a New Topical Anesthetic Method“. Ophthal Plast Reconstr Surg. Vol 25, No 3, 2009: 173-177
2 – Non- ozone depleting vapocoolants. http://www.freepatentsonline.com/6737041.html
3 – Thompson et al. “Antibacterial activity of lidocaine in combination with a bicarbonate buffer”. J Dermatol Surg Oncol. 1993 Mar;19(3):216-20.
4 – Bainbridge LC. “Comparison of room temperature and body temperature local anaesthetic solutions.” Br J Plast Surg. 1991 Feb-Mar;44(2):147-8.
5 – Scarfone RJ, Jasani M, Gracely EJ. “Pain of local anesthetics: rate of administration and buffering“. Ann Emerg Med. 1998 Jan;31(1):36-40.



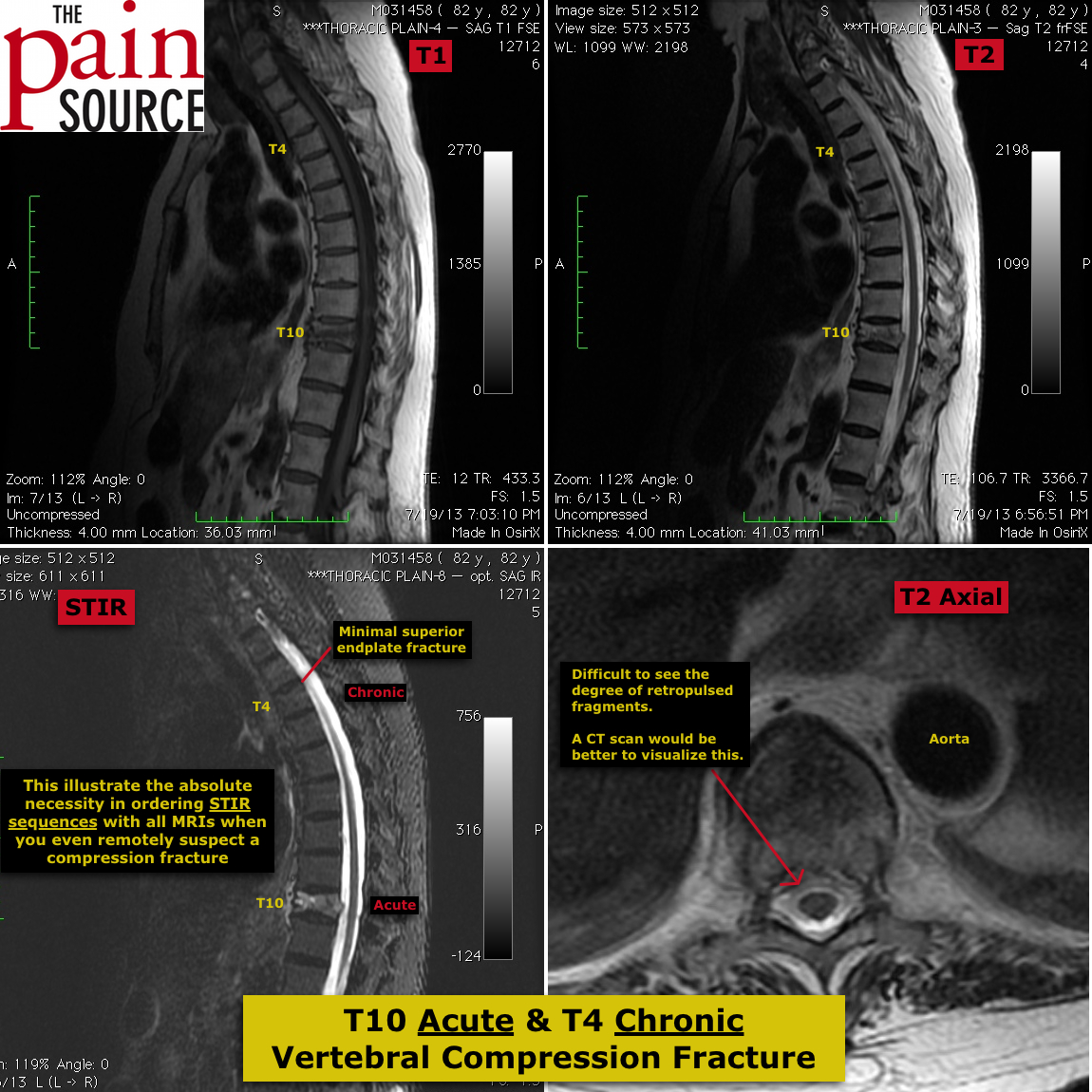




We use EMLA cream in our botox clinic very frequently. We use a pea size amount of the cream and use a duoderm dressing to help it stay in place. Most patients report excellent analgesic result after 30 minutes of application.
Then no numbing spray after the EMLA? What do you use for peripheral joint injections?
We use Ethyl Chloride spray as well. For most peripheral joint injections the EMLA + Ethyl Chloride combination works well. But usually there is not enough time in clinic to wait for the EMLA to kick in so we just use the Ethyl Chloride.