aka. “serotonin toxicity”, “serotonin storm”, “serotonin sickness”
An important adverse drug effect that is relevant to our field of pain medicine, because many of the medications that can cause this are either prescribed by us, or those which our patient population is also taking (antidepressants).
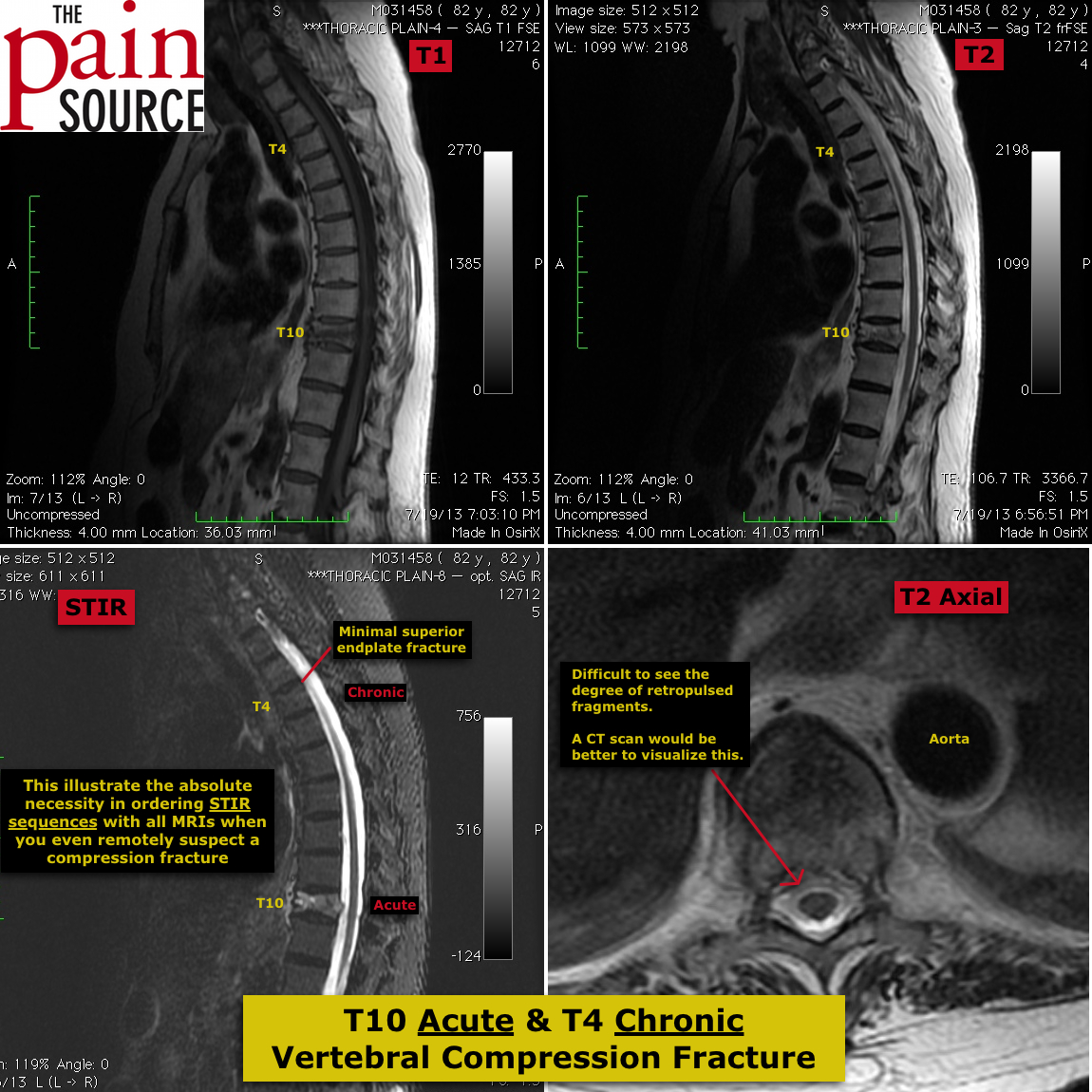
A potentially life-threatening adverse drug effect (usually a drug-drug synergistic effect) due to excessive serotonergic activity in the CNS and PNS.
- Can occur within minutes
- Mild symptoms: tachycardia, shivering, sweating, dilated pupils, myoclonus, hyperreflexia, increased muscle tone (think sympathetic)
- Moderate: hyperthermia, overactive bowel sounds, hypertension, agitation, mental confusion, hallucinations
- Severe: higher tachycardia, higher hypertension, higher temperature (106 F), seizures, renal failure, rhabdomyolysis.
- Made by signs and symptoms above, and looking at the patient’s list of medications.
- Ask the patient about medications started or dosages increased recently.
- No diagnostic tests
Treatment
- Discontinuing some medications that may be causing this.
- This is essentially a medical emergency and needs to be managed in a hospital (even though mild cases that just began may improve with discontinuation of the serotonergic medications).
- Here is a case report and explanation of serotonin syndrome, the diagnosis, and the treatment. Click here
- Cyclobenzaprine, tramadol, SSRIs, MAOIs, triptans, trazodone, opioids (esp. meperidine, fentanyl), CNS stimulants (methylphenidate).
- Remember natural supplements like St. John’s Wort and tryptophan too.
- Some of the above are a minor risk to combine (like tramadol and cyclobenzaprine), whereas others are more risky (SSRI with a SNRI)
As pain physicians, we need to be aware of this unfortunate adverse effect and be able to warn our patients of what to look out for.
Also, our office staff needs to be educated enough to make a preliminary diagnosis over the phone, recognize the emergent need for medical help, and inform us immediately.